
Can Acid Reflux Cause Chest Pain?
- Chest pain is a classic symptom of acid reflux, usually felt as a burning pain behind the breastbone.
- The burning sensation in the chest may begin in the upper abdomen and may radiate upward to the neck. Heartburn may last momentarily, but it can continue for a few hours.
- Chest pain is a symptom of various conditions, some life-threatening. It should never be self-diagnosed.
Jump Ahead
- What Is Acid Reflux/GER
- Chest Pain and Acid Reflux
- Chest Pain Has a Variety of Causes
- Warning Signs That Chest Pain May Be Serious
- Glossary of Terms
- Expert Opinion
- Resources
What Is Acid Reflux/GER

Acid reflux, also known as gastroesophageal reflux (GER), happens when the lower esophageal sphincter (LES), the ring of muscle that keeps the esophagus (food tube) closed, relaxes too frequently. Increased amounts of stomach acid and other liquids that the body makes to help digest food back up into the lower part of the esophagus causing a burning pain in the chest. Certain foods like chocolate, citrus, and greasy or spicy foods often worsen GER. [1]
Practically everyone gets “heartburn” or “acid indigestion” from time to time, but two or more times a week may indicate that a person has gastroesophageal reflux disease (GERD). [2]
Chest Pain and Acid Reflux
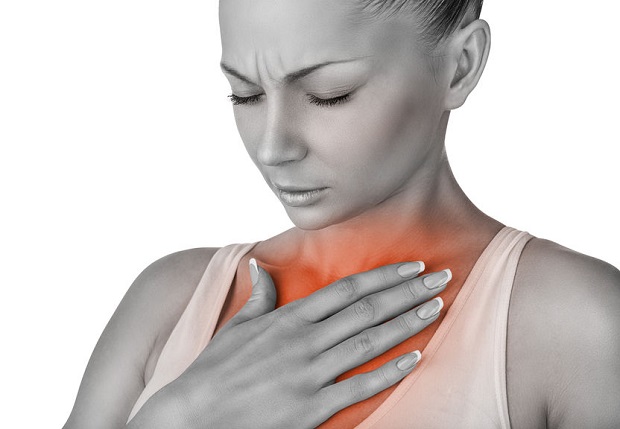
A burning sensation in the chest is a classic symptom of acid reflux, but chest pain is also a symptom of other conditions, some life-threatening. Acid reflux can occur anytime, but certain factors increase the likelihood of an attack. It usually occurs after eating, lying down, or bending over. You may have a sour taste in your mouth, especially when lying down. The burning sensation in the chest may begin in the upper abdomen and may radiate upward to the neck. Heartburn may last momentarily, but it can continue for a few hours. [3]
Chest Pain Has a Variety of Causes

If you need convincing that a physician should always diagnose chest pain, consider that any organ in the chest can cause chest pain. As well as acid reflux, it can be a symptom of other gastrointestinal disorders such as gastritis, hiatal hernia, peptic ulcer, a muscle spasm in the esophagus, and a gallbladder attack. Chest pain can also be a symptom of lung problems such as a blood clot, lung collapse, pneumonia, and swelling of the lung’s lining. It can be a symptom of shingles or strain of the muscles and tendons between the ribs. It can even be a symptom of a panic attack. [4]
It is also a classic sign of a heart attack.
Warning Signs that Chest Pain May Be Serious
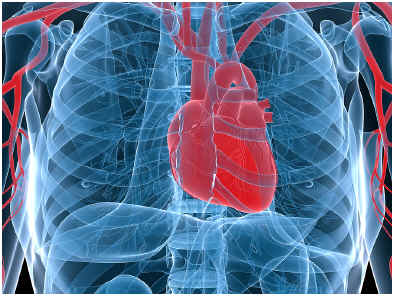
A heart attack can present with many different symptoms for different people, making it nearly impossible to tell what’s causing your chest pain, another reason not to self-diagnose. According to the Ohio State University Medical Center, there are some common warning signs of a heart attack, though individuals may experience different symptoms.
Chest pain may be a warning sign if you experience severe pressure, fullness, squeezing, or pain/discomfort in the center of the chest that lasts for more than a few minutes; The chest pain spreads to the shoulders, neck, arms, or jaw; The chest pain increases in intensity and is not relieved by rest or taking nitroglycerin. [5]
Also, note any chest pain that occurs with sweating, cool, clammy skin, paleness, shortness of breath, nausea or vomiting, dizziness or fainting, unexplained weakness or fatigue, or a rapid or irregular pulse could be a warning sign. [6]
Glossary of Terms

- Angina: Chest pain caused by reduced blood flow to the heart muscle.
- Aortic Dissection: A tear in the wall of the aorta.
- Costochondritis: Inflammation where the ribs join the breastbone or sternum.
- Pericarditis: Inflammation in the sac that surrounds the heart.
- Pulmonary Embolism: A blood clot in the lung.
- Pneumothorax: Collapse of the lung.
- Pleurisy: Swelling around the lining of the lung.
Expert Opinion

“The number of noninjury ED visits made by persons aged 18 and over complaining of chest pain or abdominal pain rose from 1999 through 2008, but the proportion of those visits with a serious diagnosis did not increase. In fact, the percentage of visits for chest pain resulting in a diagnosis of ACS decreased, consistent with reported declines in hospitalizations for acute myocardial infarction.”
Emergency Department Visits for Chest Pain… CDC
Resources
- [1] [2] WebMD – “What Is Acid Reflux Disease?“
- [3] Mayo Clinic – “Heartburn or Chest Pain: When Is it a Heart Attack?“
- [4] US National Library of Medicine-National Institutes of Health – “Chest Pain.”
- [5] [6] Ohio State University Medical Center – “Chest Pain/Heart Attack Symptoms.”
DISCLAIMER: THIS WEBSITE DOES NOT PROVIDE MEDICAL ADVICE
The information, including but not limited to text, graphics, images, and other material on this website, is for informational purposes only. No material on this site is intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified healthcare providers with any questions you may have regarding a medical condition or treatment before undertaking a new healthcare regimen, and never disregard professional medical advice or delay in seeking it because of something you have read on this or any other website.





